For many years, as an attempt to provide a natural appearance after hair transplantation was introduced by Nordstrom” and Marritt 17 in 1981 and 1984, respectively. Their primary objective was to camouflage scars and the unnatural appearance caused by conventional techniques, such as punch grafts and flaps. This was extremely time consuming, and at that time it was unthinkable to do more than just the hairline.
The use of micrografts (grafts with one or two hairs) and minigrafts (grafts with three or four hairs) in large numbers per session to cover the entire area of baldness was introduced by Uebel as early as 1986, 18,19 and demonstrated natural results with minimal scarring.
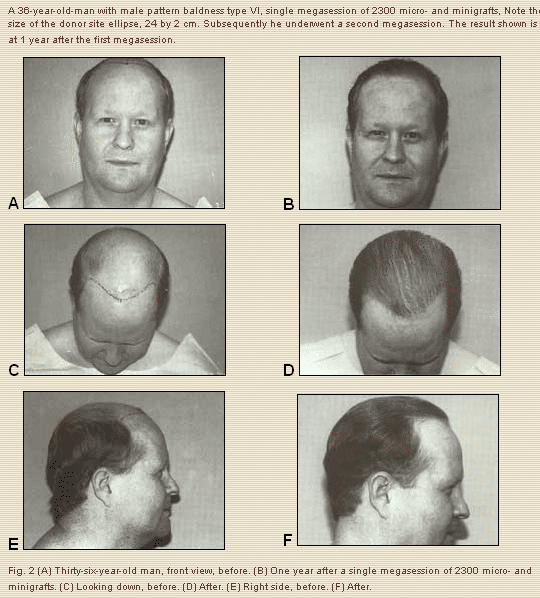
Inspired by the work of Uebel, over the past several years I have been performing micro- and minigraft megasessions. In a megasession, over 1000 grafts are done in a single session in an effort to obtain a natural result with minimal scarring, and minimal downtime. Today most megasessions I perform consist of 1500 to 2000 grafts, with 2500 as an upper limit.
The perfect solution for the treatment of male pattern baldness does not yet exist, but having personally performed over 150 such procedures, and having undergone the procedure twice myself, I feel comfortable saying that the micro- and minigraft megasession is a safe and predictable procedure, provides natural results, and requires minimal downtime (just one or two sessions). It has the added advantages of minimal scarring, and a high level of patient satisfaction. The main limitation of this procedure is the less than ideal degree of hair density. However, when properly performed it is acceptable, especially when done a second time.
As with any other procedure, time needs to be spent with the patient to make certain he understands the options and has realistic expectations. I have found that patients in their late 30s and older are glad to accept the less than ideal degree of hair density obtained by the micro- and minigraft megasession, in view of the procedure’s accompanying advantages of natural appearance, minimal scarring, and the fact that the job is completed in just one or two sessions. The younger patient (< 30 years old) usually is more demanding, and wants a density comparable to that of the donor site, which obviously cannot be obtained with this technique. In this age group, extreme caution should be exercised utilizing any technique, as it is impossible to determine the degree of hair loss that these individuals will eventually develop.
A key factor to successful hair restoration surgery is the donor dominance concept described by Orentreich, namely, that each individual hair follicle contains its own unique genetic makeup; thus, if a follicle is transplanted, it will maintain its original genetic properties regardless of the transplantation site. This has been demonstrated for almost four decades by traditional punch grafts; the transplanted hair will continue to grow in the new location, as long as it was going to do so in the site of origin.”
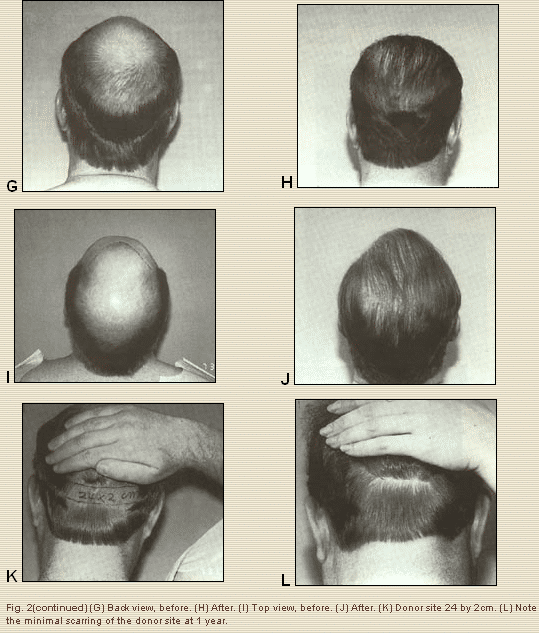
Unfortunately, once hair loss starts, it never really stops. We must also remember that no new hair is created with any technique: all we are doing is redistributing the existing hair in a more strategic way to provide better coverage. In a recent study reviewing 100 consecutive cases, I found a 97% satisfaction rate after a single megasession, and a very low complication rate with only 9% self-resolving ingrown hairs (cysts) and a 1% incidence of hypertrophic scar at the donor site only. This occurred in an African -American patient and responded to triamcinolone (Kenalog). There was not a single case of infection, hematoma, dehiscence, permanent numbness above the occipital scar, noticeable scars in the recipient site, or poor hair growth.”
Patient Selection
In brief, provided the general health is good, almost anyone is a candidate for micro- and minigrafts as long as there is good hair density in the donor area (occipital area).
If the affected (bald) area is not too large, and the donor area has good hair density as in most cases of male pattern baldness types II through V, and many VI, I will usually treat the entire bald area, and always with a conservative and mature hairline level, 6 to 9 cm cephalad to the upper border of the eyebrows.
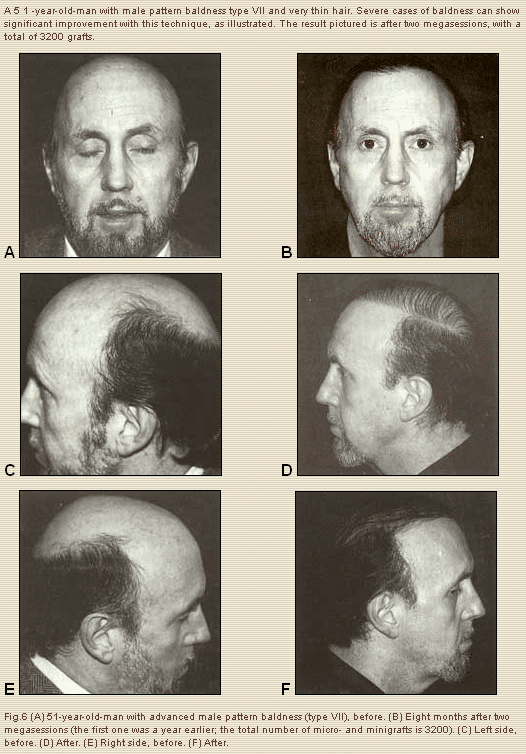
If the affected (bald) area is disproportionately large relative to the donor area (type VII baldness), one may consider transplanting only the front part of the scalp or create an isolated frontal forelock, and leave the vertex and crown bare, the main objective in this case being to frame the face. Traditionally, we have been taught that individuals with dark straight hair and light skin are poor candidates for hair transplantation, the high color contrast making grafts very obvious. Cases of blonde, light brown, gray, and red hair tend to be more forgiving, and have been considered ideal candidates, as there is less color contrast. This applies primarily to conventional round plugs and large grafts.
Using exclusively micrografts at the front 1/4 to 1/3 of an inch of the hairline provides a natural appearance regardless of skin or hair color. Curly hair tends to provide better coverage, giving the optical illusion of more hair than is actually present. However, it is more difficult to dissect the micro- and minigrafts on these individuals, because the curling also is present intradermally, and more effort and time are required for my assistants to work through such cases.
Patients whose hair is only a little wavy are not a problem at all, and their hair is as easy to dissect as straight hair. Dissection of micro- and minigrafts is difficult in patients with light colored hair (blonde and especially white hair), as it is harder to see the hair shafts and bulbs, thus requiring more time, magnification, and excellent lighting. In this cases we have found background light very helpful, as cutting on an X-ray or transparency (slide) view box with a sterile translucent surface.
Women tend to have a more diffuse hair loss pattern, which makes them generally not such good candidates for hair restoration surgery, with any technique. In reconstructive cases such as trauma, oncologic resections, and burns alopecia, the use of scalp flaps and tissue expansion would usually be better choices.
Technique Surgical Team
We have a four-person surgical team. Two of them specialize in carefully dissecting the grafts with 3.5 loupe magnification, and the other two (a surgical RN and myself) insert the grafts. So far, I have inserted every graft on all of my patients. Today we are able to cut and insert up to 600 grafts per hour, “up to” because as with any procedure the speed is a function of various factors. Generally our OR time to do 1000 grafts is about 31/2 hours; to do 1500 about 41/2 hours; and to do 2000 to 2500, about 6 to 7 hours. We estimate that at least 90% to 95% of each graft ends up growing healthy hair.
Sedation and Local Anesthesia
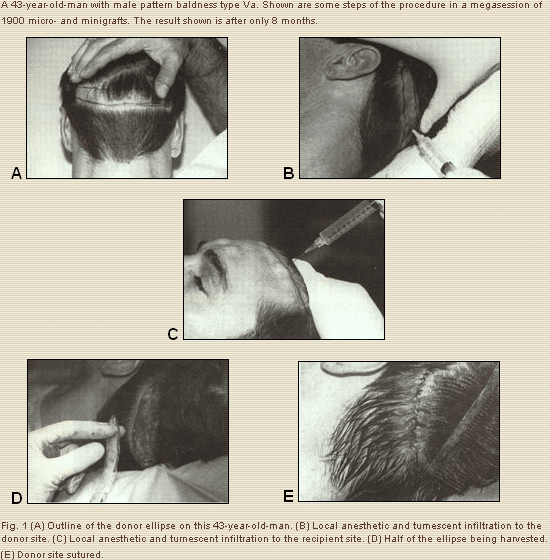
With the patient in the supine position, intravenous sedation is administered, with midazolam (Versed) and fentanyl citrate (Sublimaze). Prophylactically, we administer a gram of Ancef (cefazolin sodium) i.v. push, or if allergic, an alternative antibiotic is given such as Cipro (ciprofloxacin), 400 mg. For local anesthesia we use bupivacaine (Marcainc) 0.5% with epinephrine 1: 200,000 (approximately 40 cm3) to block the supraorbital, supratrochlear, and occipital nerves. Subsequently, tumescence is induced in both the donor and recipient areas with 0.5% Xylocaine (lidocaine) with 1:200,000 epinephrine (usually we use a total of about 150 cm3). (See Figs.1B, C.)
Donor Site
The size of the donor occipital ellipse depends on the number of grafts to be made and the degree of hair density of the donor area, and will range from 10 to 25 cm by 1. 5 to 2 cm wide (Fig. 1A). With the patient’s head turned to the left, I first harvest the right half of the ellipse using a #10 blade, and it is immediately handed to my assistants to start making grafts. Careful dissection is done parallel to the hair shafts, and also to preserve the occipital nerves and arteries.
We then undermine carefully and do a single layer closure with several interrupted, and then a simple running “3-0” Prolene suture. The patient’s head is then turned to the right to harvest the left half of the ellipse (Fig.1D). Personna prep blades or #22 blades are used to cut the grafts over a solid synthetic or wooden board; tongue blades can also be used (Figs. 1F, G). The donor ellipse and the grafts are kept chilled in normal saline, at about 4? C In addition, the grafts must be gently handled and kept wet at all times, to keep them viable. A damaged seed will grow nothing!
Graft Count and Insertion
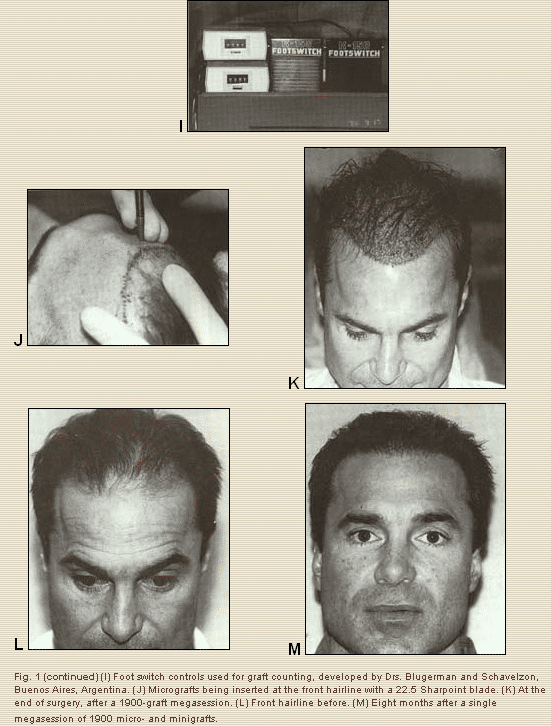
Using a foot control switch (Fig. II) the grafts are counted as they are being cut, or they can be lined up in rows and counted prior to insertion. I feel it is important to count them for several reasons: it gives you a point of reference for later objective comparison. In addition, it helps to distribute in a more strategic fashion the grafts that are available for transplantation in a given megasession. For example, suppose you have inserted 1150 grafts and your assistants indicate to you that the final count is 2020 grafts. Knowing this helps you plan and distribute wisely what you have left, establishing more or less emphasis in certain areas, such as the anterior hairline, or the parting of the hair, where we pack the grafts as densely as feasible. Further posteriorly, where it is less important, fewer grafts may be inserted.
Once tumescence has been induced with 0.5% Xylocaine (lidocaine) with 1:200,000 epinephrine, we use a 22.5 Sharpoint blade immediately inserting grafts with jewelers’ forceps at the hairline (Fig. 1J), and posterior to that we use either a 65 Beaver miniblade or a Feather I I blade. No dilators are needed, and no tissue is removed from the recipient site.
We start at the hairline, using exclusively micrografts, usually 300 to 400 are inserted in the very front, and we then proceed posteriorly, with a mixture of micro- and minigrafts, mostly minigrafts, the remaining 1200 to 2000 grafts (Fig 1 K). The grafts are initially inserted 4 to 5 mm from each other. As the fibrinogen turns into fibrin, the grafts become more secure to the recipient slits; this phenomenon allow us to place grafts closer to each other (dense packing), minimizing the popping out effect. Periodically, every 20 minutes or so, we go back anteriorly and place grafts between those inserted earlier; this allows us to accomplish the desired dense packing of grafts. The closest we have been able to insert grafts is about 1.5 mm from each other. This is critical for obtaining an acceptable degree of density and is a must for the front hairline.
Eight months to a year later, when the healing is complete and the scalp has totally recovered, a megasession may be repeated to increase density if desired; this time the grafts are placed between those of the first megasession. If the grafts are inserted very close to one another (2 mm or so) before the fibrinogen turns into fibrin, the grafts will not be secure enough and will pop out: as you insert one, one or two or even more pop out, a very frustrating experience. This is minimized by following the above-mentioned steps.
In cases of over 1500 grafts (the majority), we take a short lunch break (the patient also eats), rest for a few moments, and then go ahead and continue until all of the grafts are in. As needed, a spray bottle containing equal volumes of normal saline and hydrogen peroxide is used to keep the scalp clean. A protective dressing is applied with Adaptic, followed by a wet Kerlix, then a dry Kerlix, and finally an elastic (Ace) bandage.
Postoperative Care
The bandage is removed at 48 hours, and daily gentle shampooing is then begun. Elevation of the head of the bed is suggested to expedite disappear acne of the edema, which is in great part related to the turnescent infiltration, and is most noticeable on postoperative days 2 through 6; almost invariably, it disappears completely by postoperative day 7.
The patients are prescribed Keflex 500 mg po, qid, or Cipro 500 mg PO, bid for 3 days. Usually there is no pain at all in the recipient site; the only source of pain is the donor site, and it is easily controlled with acetaminophen and codeine and lasts only a few days. I know this personally, as I have had the procedure done twice on me.
Above the occipital suture line, paresthesia and hypesthesia normally occur for the first few weeks or months postoperatively, just as after a rhytidectomy, or a coronal forehead lift. The transplanted grafts start growing hair immediately, but at about 8 to 30 days many of them go into telogen (rest phase) and shed the hair; this is normal and occurs in almost every case and involves 50% to 90% of the grafts. At 3 to 4 months the grafts shift into anagen (growth phase) and start growing hair again.
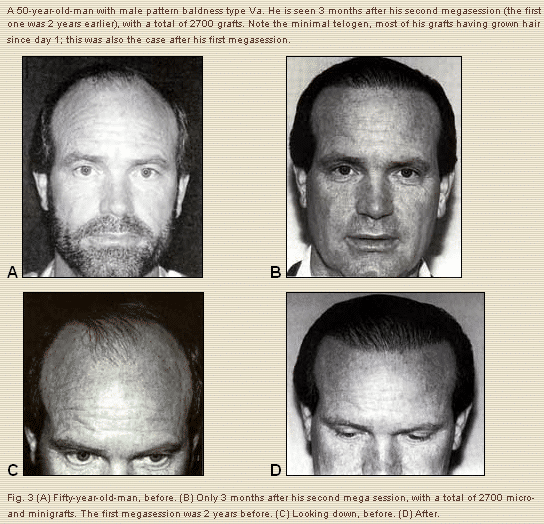
In rare cases (1% to 2% of patients), most of the grafts continue in anagen, with only a few grafts going into telogen, resulting in stable hair growth from day 1 for the majority of the grafts. By postoperative month 6, most patients show a significant improvement in terms of hair growth; however, it takes about a year for the final result to occur, after which a decision can be made as to the need for another megasession.
Examples

Discussion
Because of the procedures natural results and safety, in recent years the trend in hair restoration surgery has been toward smaller and more numerous grafts per session 21 -24.
It is important for surgeons to be familiar with the various techniques that are available for the management of any surgical challenge. There are cases in which we may need to combine techniques, to better serve our patients. This certainly applies to hair restoration surgery. The various techniques should be discussed with prospective patients. However, we also are obligated to help them select a procedure that best their needs, keeping in mind the risks and benefits involved, advantages and disadvantages, and the estimated number of procedures required. A well informed patient is the best patient.
The micro- and minigraft megasession technique described above, in my opinion, follows more closely than any other technique the criteria mentioned, namely, predictability, safety, very low incidence of complication, minimal downtime, minimal number of procedures required, minimal scarring, and a natural result both short and long term.
By “long term” results achieved with this technique, I mean that the hair distribution follows a pattern more closely resembling the one that normally occurs, that is, without clumps of hair, or blocks of hair from flaps, and without noticeable scarring. If the patient goes on to lose more of his hair, which will occur, or loses all of his hair, clearly he would look more natural having had the procedure with the micro- and minigraft megasession as described, than if he had any other technique available today.
In my experience, most patients in their late 30s and older readily accept the less than ideal degree of hair density obtained with the micro- and minigraft megasession technique, in view of the advantages realized, such as the natural appearance, minimal scarring, and the fact that in just one or two sessions the job is completed.
The density can be improved up to a point via a second megasession. And in certain cases even a third one may be done. So far, I have done three megasessions for only two patients, each time achieving greater density. However, I don’t believe that any greater density can be realized with fourth or further megasessions.
Another advantage of this procedure is that even if it is done only once, the patient looks natural, and he does not have to be committed to an endless number of procedures. We are all too familiar with the scars, the multiple procedures required, and the unnatural appearance, in some cases the temporary grotesque deformity, as well as the higher risk of complications that are associated with most of the other techniques of hair restoration surgery.
Conclusions
I am convinced that for the patient seeking esthetic hair restoration surgery, the micro- and minigraft megasession technique is an excellent option. I have found it to be safe, predictable, requires minimal downtime and minimal number of procedures, results in minimal scarring, and best of all provides natural results even in a single session. The hair density this procedure provides, although limited, is acceptable and esthetically pleasing to the overwhelming majority of patients, including myself.
Alfonso Barrera, M.D.
West Houston Plastic Surgery Clinic, P.A.
915 Gessner Rd., Suite 825
Houston, TX 77024
